The 2025 nomination round has been launched in the Central Jersey Community Choice Awards, and we ask for your support!
Visit this link and follow the instructions below. Vote through June 30th! That’s it! We appreciate your support!
Central Jersey Community Choice Awards 2025
To Nominate Belle Mead Animal Hospital
- Navigate to the Pets Category, Veterinary Hospital
- In the Nomination Field, type in Belle Mead Animal Hospital (to help us get nominated)
- Proceed to the Pets and People Category, and type in your favorite Veterinarian’s Name
- On your first visit, complete the registration with YOUR information and click “NOMINATE.”
- Continue to nominate in other categories of your own choice. Nominations are recorded as they are entered and there is no final “SUBMIT” button.
- On future visits, after your first one, log in to the ballot using the “Already Entered” function and nominate again up to once a day.
GREAT NEWS for all our RABBIT patients! We are now able to stock individual doses of the Rabbit Hemorrhagic Disease vaccine! This means that STARTING IN JUNE 2025 we will be able to schedule rabbits for vaccines during regular appointments instead of during rabbit clinics. All rabbits need to be up to date on their annual examination, and this cannot be given by technicians at tech appointments.

Rabbit hemorrhagic disease is a highly contagious, fatal disease in rabbits. RHDV2 DOES NOT affect humans, but it can affect both domestic AND wild rabbits. Infected rabbits may develop a fever, be hesitant to eat, or show respiratory signs, neurologic signs, or internal bleeding. However, many times, the only sign of the disease is sudden death.
Belle Mead Animal Hospital, Your Other Family Doctors

Come join us at PAWS IN THE PARK – 3k Run/Walk at Woodfield Park in Hillsborough, New Jersey on Monday, May 26th! Belle Mead Animal Hospital is one of the sponsors along with a few others in the community, and we would all love to have you join us there to support a worthy cause! Proceeds from the event will benefit Project K9 Hero, a 501(c)3 organization. We will have a table to meet and greet you!

If you don’t have a dog to walk with, you can still join us and go by yourself or with friends and family members. You can even simply make a donation direct to support the cause on the website link below.
We encourage all walkers, joggers, and runners who enjoy the outdoors to come out on this Memorial holiday weekend Monday for some fun and friendly community time. Participants are welcome to track their own speeds, though times won’t be published. This is meant to be a light-hearted and non-competitive event.
This run/walk has a rolling start, so come anytime between 10am-12pm to participate! Dogs must be leashed. And this is a rain or shine event, although we are expecting nice weather! More details and sign-up form here: Paws In the Park Hillsborough NJ Sign Up
We look forward to seeing you!
Belle Mead Animal Hospital, Your Other Family Doctors
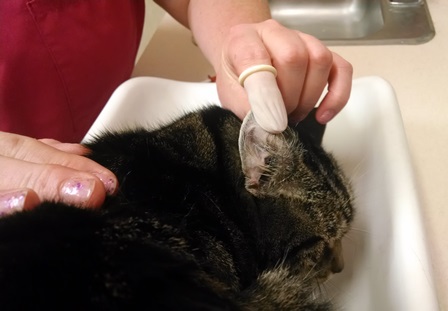
Meet Toby! He is the nicest and the cutest indoor/outdoor cat. He did so well at BMAH getting his blood work and his annual feline leukemia and rabies vaccines.
His owners love him very much, and he loves the outdoors. So the deal that they made with their cat is they will let him out during the day, but he will be wearing a Seresto flea and tick collar so that he’s protected against all the diseases that he can get outside. They will vaccinate him for feline leukemia because the vaccine is 100% effective, and he can get that just from having any interaction with another cat.

Of course, Toby is up-to-date on Rabies, but he only gets the feline rabies vaccine that a Veterinarian can give in a hospital setting. The rabies vaccine clinics that are the three-year vaccines are not recommended for cats, but they are recommended for dogs and every other species.
Indoor/outdoor cats are at higher risk for infectious diseases, rabies, bite wounds, and being hit by a car.
Totally indoor cats live nine years longer than indoor/outdoor cats on average. The reason why indoor cats live longer is because of all the reasons I listed above, therefore, they typically go to the veterinarian more often as well. However, if you make a deal with your outdoor cat, they can live just as long and do just as well.
Here is the deal: We will keep you protected from fleas, ticks, parasites and infectious disease by vaccinating you at the veterinarian and seeing the veterinarian once a year.
The other really important part of this deal is at night. When you come in for dinner, before it gets dark, so before dusk, you will stay in our home protected the entire night.
If you can make this deal with your cat, then their chances of getting hit by a car or getting a bite wound or getting a more serious disease is greatly neutralized.
Have you ever seen a dead cat in the road that was hit by a car overnight? The reason that cat was hit by a car was not because it forgot to stop and look both ways before crossing! The reason that cat was hit by a car because at night time when it’s dark, and in the cover of darkness, there are hundreds of other feral cats and animals that you will not see in the daytime. These other cats and animals will chase any cat in the middle of the night trying to breed or fight with them, and in a panic, when they’re running across the road, this is when they are most likely to get hit.
So again, completely indoor cats live longer and have fewer risks than cats that go outdoors. However, cats who are going outside, if they are kept indoors at night, have a much higher chance of being protected, staying safe and living longer.
That’s the deal! We Love Cats at Belle Mead Animal Hospital!
Dr. Joe Martins, DVM, Belle Mead Animal Hospital, Your Other Family Doctors

A client of mine who has two cats comes in every year faithfully for their annual wellness exam. This annual exam includes a weight check, looking at the teeth, listening to the heart and chest, and sometimes annual bloodwork. All this is along with conversations over any concerns, and updating their cats’ vaccines.
She called to schedule their appointment, but she said they didn’t need the rabies shots this year because they got it done for free at the January town clinic this year, just a few weeks prior to this visit.
“Oh no!” I immediately thought, because it was a “cat” at the town rabies clinic. This is scary on multiple levels.

If their pet would have been a dog, then a three-year town rabies vaccine is fine, but because it’s a cat, there is a risk that a free rabies three-year shot from the town clinic can cause cancer in some cats. For the last 50 years, we have used this three-year rabies vaccines in cats, dogs, horses, sheep, goats, pigs, and the list goes on.
About 17 years ago, in cats and only cats, we began noticing that the three-year rabies vaccine can induce a tumor at or near the injection site anywhere from two months to two years after it was given. These tumors were incredibly aggressive and used to be surgically removed by the pet’s veterinarian.
Many times these tumors were so aggressive that they would come back in the same area and usually in deeper tissue, starting to attach to the pet’s muscles and nerves. This would normally prompt the owner to come back to the veterinarian. Then the veterinarian would send them to board veterinary surgeons which were more expensive and more aggressive in the removal of these tumors. Many of these tumors, unfollowed, would still come back in a relatively short amount of time. They all inevitably caused extra pain and discomfort to the pet, and could eventually be fatal to the pet.
Other things that were done to try and slow down regrowth of these tumors and give these animals more time were to send these cats to specialists for second and third opinions. The newest treatment recommendations back then was to not decide on a quick surgery first, but to see a specialist. They started recommending that these pets get a biopsy and see a specialist for radiation to kill every microscopic cell possible to decrease the chance of it coming back, or at least the plan was to try and get a cure to decrease the time interval as well.

So as a young Veterinarian starting a career 27 years ago, the Rabies vaccination was very important to protect all pets and all animals. The Coincidence was that this life-saving vaccine that was designed to save pets was actually now a cause for alarm. Back in those days, no one really knew that this was going on for a while because pets and humans got all kinds of skin and under the skin cancer.
Therefore, a tumor secondary to a rabies vaccine was not on anyone’s radar. Skin and subcutaneous tumors were common, and some didn’t really grow or change for months or years. Some could be quite aggressive and grow at the injection site. Other tumors found could potentially be microscopically spreading to other organs or the chest, and we might not even know it would hurt these patients later. This is why we don’t watch a tumor for an entire year before bringing it for a veterinarian’s opinion.
I practiced for the first five years and removed many tumors from both dogs and cats. Most were not this aggressive feline cancer, but I did have a few cases of a fibro sarcoma that I removed and diagnosed with a biopsy.
Those first five years I would annually do the free Rabies Clinic for the municipality in which I lived in order to help out the community and to give free vaccinations for dogs and cats. It was a service that I thought not only protected pets, but also humans. It was really appreciated by many people. I donated my time, typically Saturday morning for free to help the community and their pets.
As more and more veterinarians were sending tumors out for histopathology and more and more similar experiences were being encountered, studies with results came out. University level studies finally realized that the Rabies three-year vaccine was inducing a tumor at the injection site in cats and only cats.
The rate of this tumor at the injection site with the rabies three-year vaccine was 1 in 10 to 20,000 cats. So we at Belle Mead Animal Hospital only give the safe feline rabies one-year vaccine that is specifically designed for cats and only cats.
Town clinics that are run by the state will not go out of their way to buy a more expensive rabies vaccine specifically designed for cats that technically only last a year. That’s fine in a few cases where you may have a farm cat or a feral cat who may never go to a veterinarian again. Their chance of getting rabies is a lot higher than not vaccinating them, so the three-year vaccine may be best in that case. However, in my opinion, for mostly indoor pet cats, the vaccine of choice is the one-year rabies vaccine designed only for cats you can only get from a veterinarian, not a town municipality. Sometimes you get what you pay for, and in this case, “free” is not good for cats when it comes to rabies vaccine clinics.
So if you want to protect cats, then make sure that they go to their veterinarian for rabies vaccines and not rabies clinics.
Dr. Joseph Martins, DVM, Belle Mead Animal Hospital

The Book Fair Family Night at the Woodfern Elementary School in Hillsborough, New Jersey was so much fun on Wednesday, March 5, 2025! Belle Mead Animal Hospital was honored to participate this year.
There was a full schedule of activities planned, from children reading the therapy dogs, to local business personalities reading to the children. Our own Dr. White had a wonderful time teaching the children a little about the day in a veterinarian’s life and reading to them.


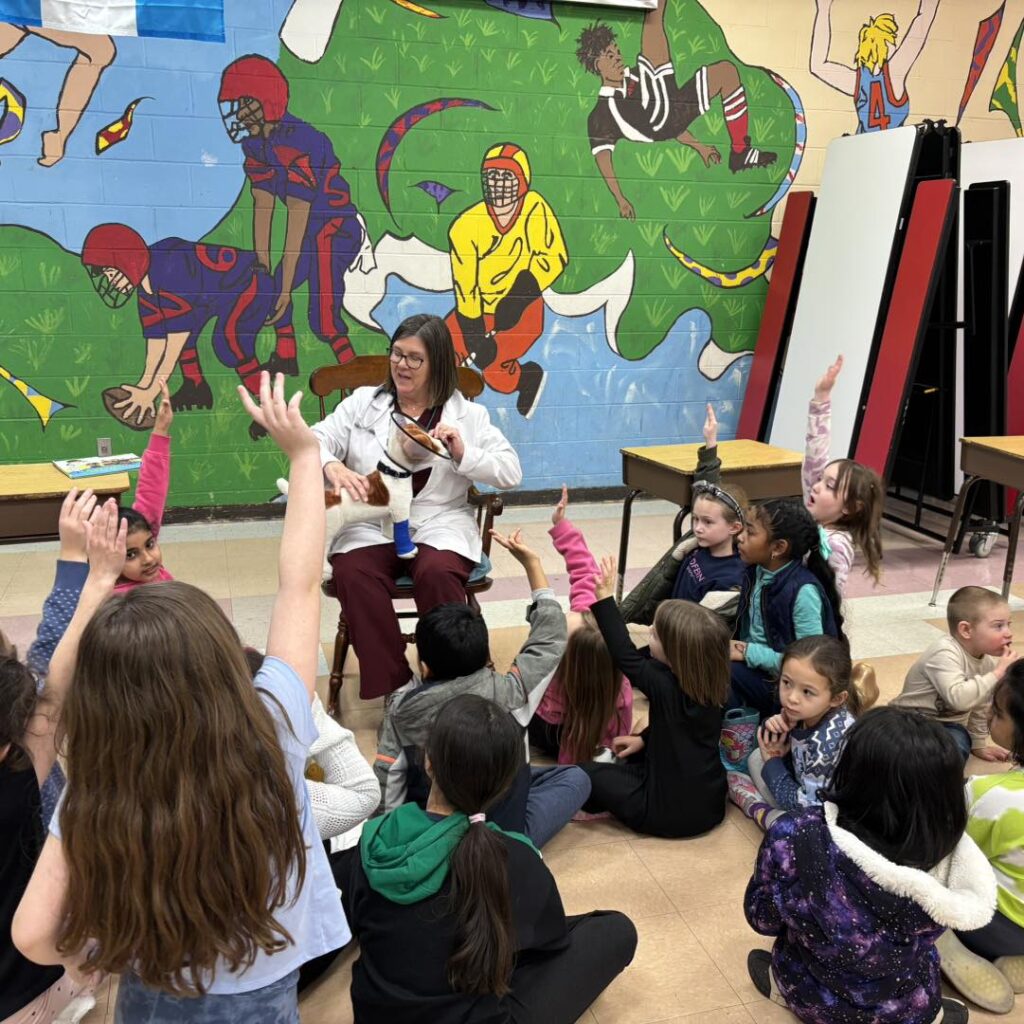
Special Guest Readings to the children included:
6:00pm: Read with Dr. Kerrigan—our Top-Dog of the night!
6:15pm: Firefighter & Dalmatian Rescue tales—woof!
6:30pm: Dog Groomer tales—getting the fur real scoop!
6:45pm: A ruff job, but someone’s gotta do it—read with a Working Police Dog Unit!
7:00pm: Dr. White from Belle Mead Animal Hospital talks vet life!
7:30pm: Gail & Rip from Make Sit Happen—sit, stay, and listen to some paw-some service dog adventures!
There was a special Adopt a Dalmatian stuffed animal, courtesy of Hillsborough Fire Department, for the first 50 kids! Bingo activities were also planned during the evening.
Let’s not forget the raffles! Belle Mead Animal Hospital was happy to donate an Amazon Kindle Reader for the raffle grand prize! We hear it was much appreciated by the winner!
Thanks to all the kids who reminded their grownups to bring in old blankets and towels or a can of dog/cat food for donation to a local animal shelter in need. Belle Mead Animal Hospital was able to collect part of the donation to pass along to a local animal rescue group. Your donations were greatly appreciated!
It was an awesome evening for people and pets. We are so happy to have been a part of it.
Belle Mead Animal Hospital, Your Other Family Doctors
Rabies is a very serious viral infection of the central nervous system (brain and spinal cord) that can affect all warm-blooded animals. The virus is excreted in the saliva of an infected wild animal such as a raccoon, fox, skunk, or groundhog.
However, less commonly talked about are infected bats that inadvertently fly inside houses. Every once in a while we have a client who experiences a bat in their house that has interacted with their pet and calls us for advice.
Our suggestion is if you see a bat fly into your house through a door or window, and you are sure it has not been in contact with any person or pet in your household, you can certainly try to chase it back out as soon as possible with a long handled instrument such as a broom. Do not touch the bat. Otherwise, you can try to contain the bat in one room behind closed doors and call Animal Control for assistance.
Word of caution:
If the bat has touched any person, or if there is a chance that your cat (or dog or ferret) may have touched the bat or has been playing with it before you discovered it, do your best not to let the bat escape.
A risk assessment needs to be performed in this case to determine if the amount of contact with the bat could have been enough to transmit the rabies virus. If the answer is no, the bat can then be released. However, if the answer is yes, then it is very important to keep the bat so it can be tested for rabies. Your pet must then be quarantined as well.
Our best advice: Stay current on your pet’s rabies vaccines
Even though your cat may never go outside, the day may come when the pet escapes through an open door and gets out by accident. And in the case of bats, one entering your home is not unheard of. Even those with pet doors who allow pets in and out can be at risk if a wild animal suffering from rabies enters the home through the pet door. This also is not unheard of.
Please allow your pets (both indoor and out) to be vaccinated for rabies by a veterinarian on a regular basis. Please follow your vet’s advice to stay current and keep records. Vaccination is by far the best insurance for preventing rabies in your pets and avoiding unpleasant, long and difficult quarantine periods. If infected, once signs and symptoms of illness appear (usually 2-12 weeks following the bite), there is no cure or treatment for the disease. Better to be safe than sorry.

Recommended Reading:
Important information about Rabies from the Somerset County Department of Health
Bat Found in Dog’s Mouth in Palm Beach Gardens has Rabies
Joe Martins, DVM, Belle Mead Animal Hospital
Preparing for a business trip or family vacation? What if an emergency arises and you must leave town for an extended period of time? Who will take care of kitty while you are away?
Cats are creatures of habit, and some adjust better than others to changes of routine and scenery. Yes, pet sitters and trusted friends as caretakers can be an option so you can leave them home with no disruption, but we also highly recommend boarding cats at an animal hospital or professional cat-specific boarding facility that works closely with a veterinarian. Why?
Who knows your animal better besides you than your veterinarian and vet technicians? And a cat-specific boarding facility who works closely with a veterinarian is also typically well trained on noticing the nuances of a cat’s behavior and changes in eating habits, and they will quickly contact the pet’s veterinarian with questions and concerns before a real medical emergency arises.
We see many times well-intentioned owners who leave their cat home with a caretaker, but fail to leave them proper instructions on what to do in case of an emergency. By the time the pet parent returns home, their feline friend is in desperate need of medical care.
Many cats get depressed and dehydrated when owners leave them home alone for longer than normal lengths of time which can push them deeper into kidney and liver disease. The cat may also hide from the caretaker while in this stressed and anxious emotional state when their pet parent is gone, without the caretaker even realizing this is a problem.
Cats left alone will also become bored and frustrated. Their appetite will decrease, they will drink less water and may even chew on fabrics or objects out of the ordinary. Some will urinate and defecate where they shouldn’t, and pet parents might think this is spiteful behavior. Spite is a human emotion. Cats display this behavior as a reaction to stress and/or a medical issue.
If your cat has any health issues requiring medications or careful monitoring for problems, boarding at an animal hospital can certainly be the best choice while you are away.
When choosing a boarding facility, we suggest you take a tour of the facility ahead of time and ask lots of questions. The facility should be clean, water bowls should be full, and comfortable bedding should be provided along with adequate and clean litter boxes. Any reputable boarding facility will require that your cat’s vaccinations are up to date for their protection and will ask who to call in case of emergency.
We also advise that the pet owner leave something in writing at drop off in case of an unexpected emergency when the owner can’t be reached. This pet owner document should pre-authorize in writing what amount you are willing to spend on emergency diagnostics and care. Also be specific about things like whether you authorize CPR.
If your cat is on a special diet or a finicky eater, ask that he/she be fed the same diet, and leave that food along with special toys that make your pet feel closer to home.
If you do choose to leave your cat home under the care of a trusted sitter or friend, please be sure to leave full instructions as noted above on what to do in case of emergency. Write down the name and number of your pet’s veterinarian and nearest emergency clinic, and make yourself available for questions about the cat’s behavior while you are gone.
Some careful planning in advance will ensure kitty has a positive experience while you are away, and your trip can be worry-free where your pet is concerned.
Recommended Reading:
Why environmental enrichment is important for cats
Dr. Joe Martins, DVM, Belle Mead Animal Hospital
Once again we would like to extend our heart-felt appreciation to all our clients who voted for us in the 2024 Central Jersey Community’s Choice Awards!
Belle Mead Animal Hospital was selected as a finalist in the contest. We could not have done it without you – all of our valued clients.
We love treating your pets as if they were our own, and will continue to do our best to serve you throughout the coming year.

Belle Mead Animal Hospital, Your Other Family Doctors
A microchip is the size of a tiny piece of rice that can be inserted between the shoulder blades of a dog or a cat within seconds. We just use a special needle with a microchip at your veterinarian’s office.
We can do this on any pet at any age – awake or sedated. It’s no more painful than a shot. We typically recommend doing it young when the pet is around six months old and getting spayed or neutered. However, if that opportunity was missed, it could be done anytime. Just talk to your veterinarian hospital staff.

It’s also very affordable, less than $75, and it’s safe and a necessity for any pet who can’t advocate for themselves, which is all pets. These microchips never cause issues and usually stay under the skin right where they’re placed, between the shoulder blades. They usually work forever, so one and done. However occasionally they can migrate up or down the back or even down the leg, or occasionally they can stop working. This doesn’t cause any issues, but have your pet scanned yearly to be sure placed properly and working.
When lost pets are scanned, the entire body SHOULD be scanned, and if not found between the shoulder blades right away, then scan up and down the front legs to catch any that may have migrated. But, as a pet owner, IT IS YOUR RESPONSIBILITY AT THEIR YEARLY VET EXAM, to ask for a quick scan to make sure that: (1) the chip is still working, (2) the location of the chip is good, and (3) that the chip information is correct.
 Remember, microchips save lives and reunite families with their pets. One pet every 6 minutes is reunited with their owner in America because of a microchip. Chips are inert and safe. There are no electronics, no emitters and no radiation. It’s not a LoJack, just a chip. So when your pet gets lost because someone left the gate/door open accidentally, or the dog ran away or was stolen, it will eventually get picked up and brought to a veterinary clinic or an animal shelter. We will scan for a chip with a hand-held scanner, and within seconds we have the information you want us to know.
Remember, microchips save lives and reunite families with their pets. One pet every 6 minutes is reunited with their owner in America because of a microchip. Chips are inert and safe. There are no electronics, no emitters and no radiation. It’s not a LoJack, just a chip. So when your pet gets lost because someone left the gate/door open accidentally, or the dog ran away or was stolen, it will eventually get picked up and brought to a veterinary clinic or an animal shelter. We will scan for a chip with a hand-held scanner, and within seconds we have the information you want us to know.
For example, your name and your phone number, or your name and your address and your phone number or email. It’s something that can be changed whenever you move at no additional charge just by logging on.
If your pet ever gets lost, you can’t depend on a collar identification only. Most pets lose collars or tags while on the run. They can’t lose a microchip. When a pet is found by a stranger or a Good Samaritan, they will call the police or animal control, and the pet usually ends up in an animal shelter. A shelter that is full could potentially traumatize or euthanize your dog or cat if they are not microchipped. Protect your pets. Microchips save lives.
Joseph Martins, DVM, Belle Mead Animal Hospital